Vaccinated but vulnerable
Nigeria received meningitis vaccines to combat an outbreak, meanwhile, health minister says over 16,000 doctors emigrated, worsening the country's healthcare crisis.
Nigeria has received over one million meningitis vaccine doses from a Gavi-funded global stockpile to counter a deadly outbreak that has claimed more than 70 lives and caused over 800 infections. The vaccination campaign will begin in Kebbi and Sokoto States, with plans to extend to Yobe. The disease disproportionately affects individuals aged 1–29. Meanwhile, Coordinating Health Minister Ali Pate revealed that over 16,000 Nigerian doctors have emigrated in the past 5–7 years, citing poor conditions and better opportunities abroad. The doctor-to-population ratio now stands at 3.9 per 10,000—well below global standards—putting pressure on Nigeria’s strained healthcare system.
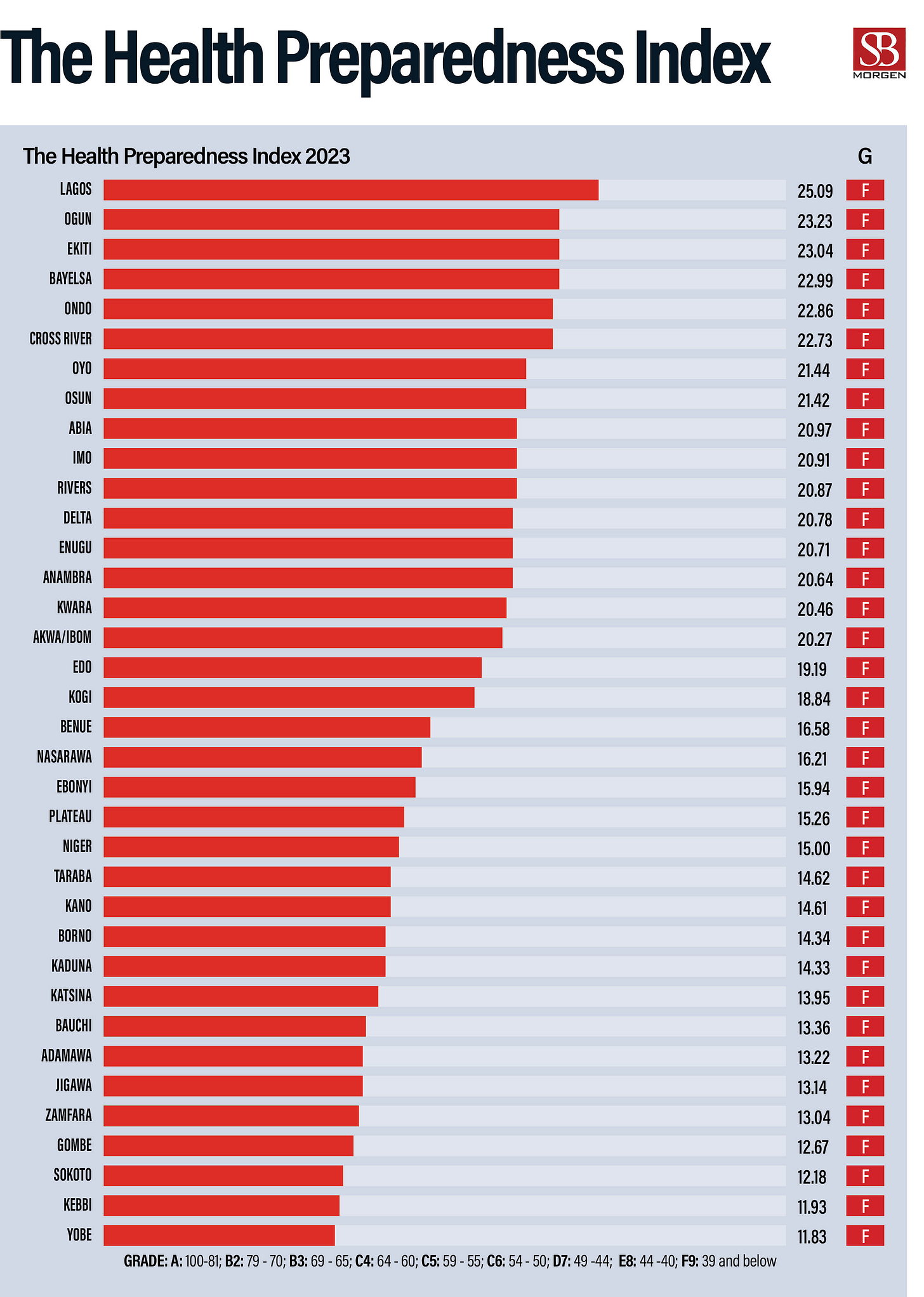
Nigeria has historically battled recurrent meningitis outbreaks, particularly in the northern regions, where the disease has had devastating effects on communities. Each year, many lives are tragically lost to this preventable illness. The growing impact of climate change, including rising temperatures and prolonged heat waves, has contributed to the increased prevalence and severity of meningitis cases. In this context, the recent delivery of over one million vaccine doses from the Gavi-funded global stockpile is a timely and critical intervention. This preventive measure will play a significant role in curbing the spread of the disease and protecting vulnerable populations. Prioritising vaccination, especially among those aged 1–29 years, who are most at risk, will save lives and strengthen Nigeria’s public health response. The planned campaign in Kebbi, Sokoto, and later Yobe States is a welcome step toward safeguarding the health and well-being of millions.
As rightly noted by Ali Pate, the Coordinating Minister of Health and Social Welfare, Nigeria is experiencing a significant brain drain, with the health sector being one of the most affected. The departure of over 16,000 doctors in the past half-decade has critically undermined the country’s healthcare system. Nigeria currently has a doctor-to-population ratio of 3.9 per 10,000, far below the World Health Organisation's recommended standard of 1 doctor per 1,000 people, presenting a clear and urgent public health crisis. As highlighted in SBM Intel's October 2024 report on Nigeria's health system, this troubling trend stems largely from poor working conditions, inadequate remuneration, and limited career advancement opportunities for medical professionals in Nigeria.
The government must prioritise reforms to improve healthcare workers' welfare and working environment. This includes competitive salaries, access to cutting-edge research and equipment, and incentives for service in underserved rural areas. Additionally, partnerships with international organisations should be leveraged for emergency aid and sustainable capacity-building. Failure to take decisive action will exacerbate the ongoing loss of healthcare personnel, increase mortality rates, and hinder Nigeria’s ability to achieve its Universal Health Coverage (UHC) goals. Retaining medical talent is a matter of national interest and a cornerstone for building a resilient and effective healthcare system.
The meningitis outbreak and doctor exodus are symptoms of the same problem: a healthcare system in distress. Without systemic change, Nigeria will continue to lurch from one health emergency to another, with preventable diseases claiming lives and medical professionals fleeing in search of stability. The government must prioritise healthcare reform—not just for crisis response but for the country’s long-term well-being.

